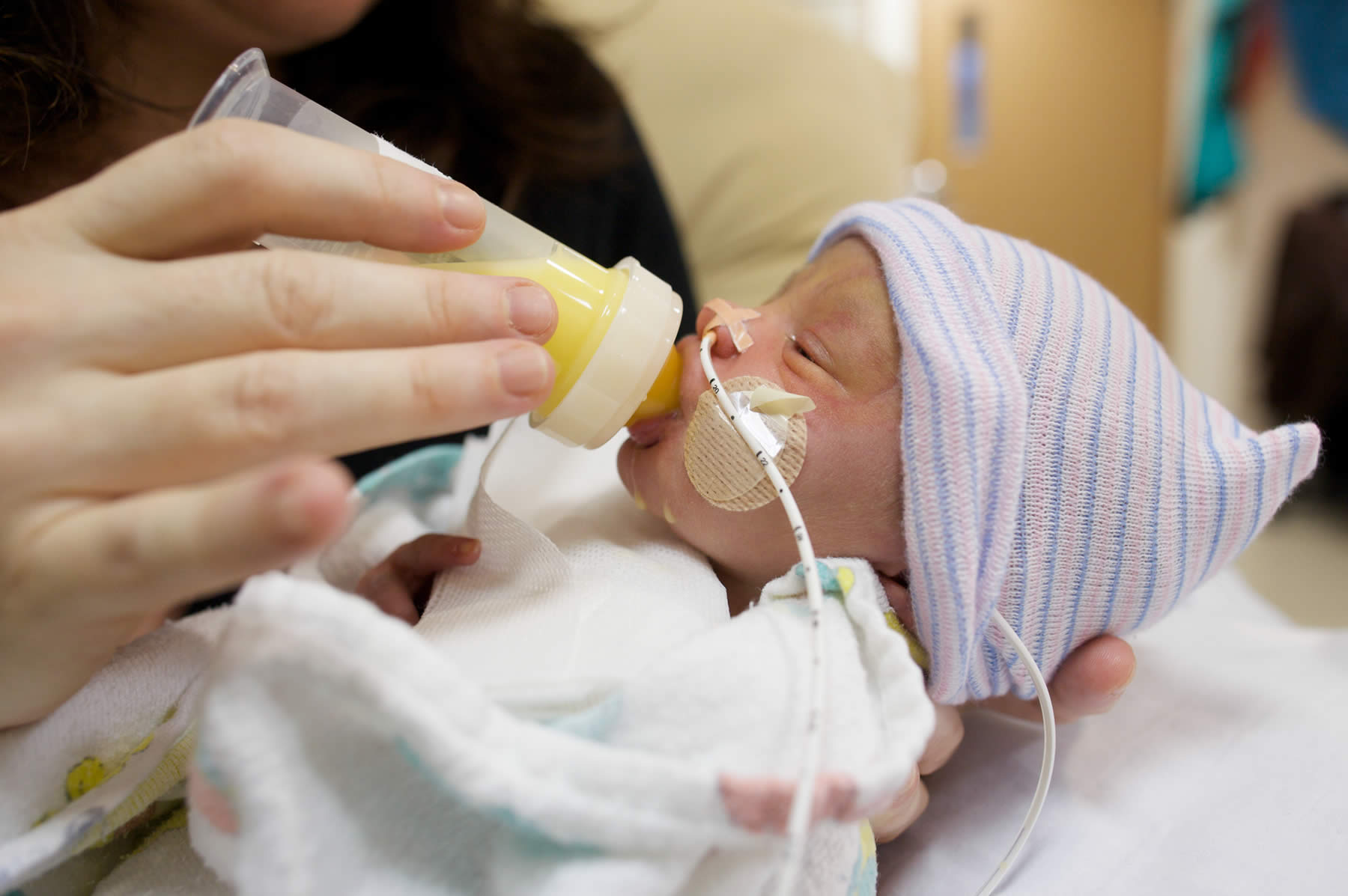
When infants have necrotizing enterocolitis (NEC), it means their intestines can’t hold waste products anymore. This often allows bacteria to pass into the baby’s bloodstream, which can lead to life-threatening infections. If a perforation in the intestinal wall occurs, bacteria can also pass into the infant’s abdomen. Babies that have a confirmed NEC diagnosis can quickly become very sick. For this reason, a doctor may need to remove any sections of dead intestine.
Immediate Complications That Can Occur After NEC Diagnosis
Even after surgical intervention, a NEC diagnosis can lead to other serious issues, such as:
- Holes in the baby’s intestines or bowel
- Intestinal scarring or strictures (narrowed passageways)
- Trouble absorbing calories and nutrients from food
- Sepsis, a type of severe infection that can affect the baby’s entire body
- Death
Why Do Some Babies Develop Necrotizing Enterocolitis?
NEC diagnosis primarily occurs among premature infants born at or before 32 gestational weeks. Despite decades of research, the condition’s root cause remains unknown. Certain risk factors associated with higher NEC diagnosis rates among infants include:
- Babies born with health problems, such as congenital heart defects
- Formula feeding
- Difficult births or babies born with low oxygen levels, since that reduces blood flow to the baby’s intestinal tract
- Very low birth weight (i.e., less than 1500 grams)
Lasting NEC Diagnosis Complications To Prepare For
About half of all NEC diagnosis babies develop long-term health complications after treatment. The two most common conditions parents should expect to deal with going forward include:
- Intestinal stricture (affects 25%-33% of NEC diagnosis babies)
- Short-gut syndrome, also known as short-bowel syndrome (affects up to 23% of babies that undergo intestinal resection surgery)
Less-common complications that may occur after NEC diagnosis include cholestatic liver disease, recurrent NEC, or metabolic complications.
Half of all babies born prematurely eventually develop some abnormalities in motor skills or intelligence during childhood. However, population studies indicate there is no direct causal link between these specific developmental issues and NEC diagnosis.
Intestinal Stricture: What to Expect
Intestinal stricture after NEC diagnosis is most common in babies that don’t require surgery to remove dead tissue. It typically occurs about one month after the child recovers from an initial NEC diagnosis and treatment regimen. The most common symptoms indicating intestinal stricture include bloody stools, failure to thrive (i.e., gain weight) and bowel obstruction. NEC babies with this long-term complication may need additional surgery or hospitalization. Thankfully, studies show NEC babies typically recover well after treatment to specifically address any resulting intestinal stricture.
Short-Gut Syndrome Treatments & Prognosis
Any NEC baby with short-gut syndrome will have difficulty absorbing enough calories and nutrients during the first two years. Dehydration is another common risk for these patients. As a result, parents should seek out pediatricians with experience treating short-gut syndrome in babies born prematurely. Children with short-gut syndrome may need the following interventions for the first few years of life:
- Parenteral nutrition. This involves infusing nutritionally complete products intravenously.
- Enteral nutrition. This is another term for a feeding tube that delivers liquid food directly into the child’s stomach.
- Supplementation with necessary vitamins and minerals. This is most common among toddlers receiving parenteral or enteral nutrition.
- Oral rehydration solutions. Since dehydration is a common risk after NEC diagnosis, drinking water alone isn’t enough. Children may need special drinks that contain salts and minerals specifically designed to prevent dehydration, such as Pedialyte.
- Special diet formulated by a nutritionist. Children that recover after NEC diagnosis are more likely to have lifelong dietary issues and suffer from reflux. Avoid any foods that tend to trigger diarrhea (i.e., high in fat, fiber, sugar, or protein). Small, frequent feedings are better for the child’s digestion. A nutritionist can provide a specific diet plan based on the individual child’s nutritional needs at every stage of development.
If you would like to learn more about negligence and the role it plays in your case, please contact Levin, Rojas, Camassar, and Reck, LLC today.